Non-Stress Test in Pregnancy: Navigating Pregnancy Care with Courage
Non-Stress Test in Pregnancy: Navigating Pregnancy Care with Courage
Introduction
Welcome to our guide on non-stress test in pregnancy—where reassurance meets empowerment, and every heartbeat tells a story of love.
Pregnancy is a remarkable journey filled with anticipation, excitement, and countless milestones along the way. As expectant mothers, we eagerly await each prenatal appointment, cherishing the opportunity to monitor our baby’s growth and well-being. Among the various prenatal assessments, non-stress test in pregnancy holds a special significance, offering valuable insights into our baby’s health and ensuring peace of mind throughout the pregnancy journey.
Join us as we unravel the mysteries of non-stress test in pregnancy, empowering you with knowledge and reassurance as you embark on this beautiful journey of motherhood. From understanding the purpose of non-stress test in pregnancy to interpreting their results and everything in between, let’s navigate this aspect of prenatal care together, ensuring the health and well-being of both you and your precious little one.
With each heartbeat, a story unfolds—a story of love, hope, and boundless joy. Let’s embark on this journey hand in hand, embracing the wonder of pregnancy and the miracle of life within.
Table of Contents
Understanding Non-Stress Test in Pregnancy
Non-stress test in pregnancy (NSTs) is a standard part of prenatal care aimed at assessing the well-being of the fetus. These tests provide valuable insights into the baby’s health by monitoring its heart rate patterns in response to its own movements. Let’s delve deeper into understanding non-stress tests and why they are an essential component of prenatal care.
Why Non-Stress Tests Are Important?
Non-stress test in pregnancy stands as a pivotal assessment during pregnancy, playing a crucial role in safeguarding the health and vitality of both the expectant mother and her baby. These tests hold paramount importance for several reasons, each contributing to the comprehensive prenatal care regimen. Let’s explore why non-stress test in pregnancy is an indispensable in the realm of obstetrics:
- Monitoring Fetal Health: Non-stress test in pregnancy provides a real-time insight into the well-being of the fetus by assessing its heart rate patterns. This continuous monitoring allows healthcare providers to gauge the baby’s response to its own movements and ensures that it receives an adequate oxygen supply from the placenta.
- Early Detection of Complications: By detecting deviations in fetal heart rate patterns, non-stress test in pregnancy can identify potential complications such as fetal distress or oxygen deprivation. Early detection enables healthcare providers to intervene promptly, minimizing the risk of adverse outcomes for both the mother and the baby.
- Risk Stratification in High-Risk Pregnancies: Non-stress tests are particularly valuable in pregnancies deemed high-risk due to factors such as gestational diabetes, preeclampsia, advanced maternal age, or a history of pregnancy complications. Regular non-stress test in pregnancy help stratify risk levels and guide personalized care plans to optimize pregnancy outcomes.
- Reassurance for Expectant Mothers: For expectant mothers, non-stress test in pregnancy offers peace of mind and reassurance about their baby’s health and well-being. The ability to monitor the baby’s movements and heart rate patterns provides tangible evidence of fetal vitality, alleviating anxiety and promoting maternal confidence.
- Timely Intervention and Management: Non-stress test in pregnancy serves as a valuable tool for obstetricians and midwives to make informed clinical decisions. In cases where non-reactive test results or concerning heart rate patterns are observed, healthcare providers can initiate timely interventions, such as additional monitoring, further testing, or expedited delivery if warranted.
In essence, non-stress test in pregnancy is instrumental in ensuring optimal prenatal care and safeguarding the health of both the expectant mother and her baby. By offering continuous monitoring, early detection of complications, and personalized management strategies, non-stress test in pregnancy plays a vital role in promoting healthy pregnancies and facilitating safe deliveries.
What to Expect During a Non-Stress Test
Non-stress test in pregnancy is a straightforward yet essential prenatal assessments designed to evaluate the well-being of the fetus. Understanding what to expect during a non-stress test can help alleviate any apprehensions and ensure a smooth experience for expectant mothers. Let’s explore the typical process and components of a non-stress test in pregnancy:
- Preparation: Before the non-stress test in pregnancy, you may be asked to eat a light meal or snack to encourage fetal movement during the test. It’s advisable to wear loose, comfortable clothing to ensure ease of movement and optimal sensor placement.
- Setting: non-stress test in pregnancy is typically conducted in a comfortable, quiet room within the obstetric clinic or hospital setting. The room will be equipped with a reclining chair or examination table where you can comfortably recline during the test.
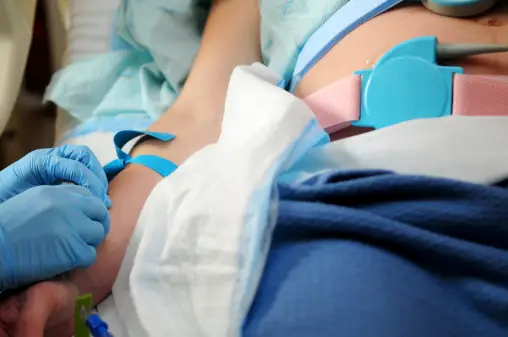
- Sensor Placement: Healthcare providers will apply two sensors to your abdomen—one to monitor the baby’s heart rate and another to record uterine contractions, if necessary. These sensors are secured with straps or adhesive patches to ensure proper contact with your skin.
- Monitoring Period: The non-stress test in pregnancy itself usually lasts between 20 to 40 minutes, although this may vary depending on the healthcare provider’s protocol and your individual circumstances. During this time, you’ll be asked to relax in a reclined position while the sensors continuously monitor the baby’s heart rate and movements.
- Fetal Movements: Throughout the test, you’ll be encouraged to pay attention to your baby’s movements and report any kicks, rolls, or other sensations you feel. Fetal movements play a crucial role in generating reactive heart rate patterns, so it’s essential to stay attentive and responsive during the monitoring period.
- Recording and Analysis: As the non-stress test in pregnancy progresses, healthcare providers will closely monitor the baby’s heart rate patterns displayed on a fetal monitor. These patterns are recorded and analyzed to assess the baby’s response to its own movements and ensure adequate oxygenation.
- Post-Test Discussion: Once the non-stress test in pregnancy is complete, your healthcare provider will review the results with you and discuss any findings or observations. In the majority of cases, a reactive NST result—with reassuring heart rate patterns—provides peace of mind and indicates a healthy, thriving baby.
By understanding what to expect during a non-stress test, you can approach the experience with confidence and actively participate in monitoring your baby’s well-being. Remember to communicate openly with your healthcare provider, ask any questions you may have, and trust in the expertise and support of your prenatal care team.
Interpreting Non-Stress Test Results
Interpreting non-stress test (NST) results is a critical aspect of prenatal care, as it provides valuable insights into the health and well-being of the fetus. Understanding how to decipher NST results empowers healthcare providers to make informed decisions and ensures optimal care for both the expectant mother and her baby. Let’s delve into the process of interpreting NST results:
- Reactive Non-Stress Test: A reactive NST result is considered reassuring and indicative of a healthy, thriving fetus. In a reactive NST, the baby’s heart rate demonstrates the expected accelerations in response to its movements. These accelerations typically involve an increase in heart rate of at least 15 beats per minute (bpm) lasting for at least 15 seconds, occurring at least twice within a 20-minute period.
- Non-Reactive Non-Stress Test: A non-reactive NST result may warrant further evaluation but does not necessarily indicate a problem with the baby’s health. A non-reactive NST occurs when the baby’s heart rate fails to demonstrate the expected accelerations in response to movements. This may be due to factors such as fetal sleep cycles, medications, or a suboptimal monitoring environment.
- Fetal Heart Rate Variability: In addition to accelerations, fetal heart rate variability (FHRV) is another crucial parameter assessed during NSTs. FHRV refers to fluctuations in the baby’s heart rate over time and is indicative of the autonomic nervous system’s integrity. Adequate FHRV suggests a well-oxygenated and neurologically intact fetus.
- Additional Considerations: Healthcare providers also consider other factors when interpreting NST results, such as the presence of uterine contractions, baseline fetal heart rate, and overall clinical context. These factors provide valuable context and may influence the interpretation of NST findings.
- Clinical Decision-Making: Based on NST results, healthcare providers may recommend additional testing or interventions to further assess fetal well-being. This may include additional monitoring, ultrasound evaluation, or expedited delivery if concerns arise. Conversely, reassuring NST results may provide peace of mind and support ongoing expectant management.
- Communication and Support: It’s essential for healthcare providers to communicate NST results clearly and compassionately with expectant mothers, addressing any questions or concerns they may have. Open dialogue fosters trust and collaboration between the healthcare team and the expectant mother, ensuring comprehensive prenatal care.
By understanding how to interpret NST results, healthcare providers can effectively assess fetal well-being, guide clinical decision-making, and provide tailored care to support a healthy pregnancy journey. Open communication, ongoing monitoring, and collaborative decision-making are key pillars of optimal prenatal care.
When Non-Stress Tests Are Recommended
Non-stress tests (NSTs) serve as valuable tools in prenatal care, providing insights into fetal well-being and guiding clinical management. While NSTs are not routinely performed for all pregnancies, certain indications prompt their recommendation to ensure comprehensive monitoring and early detection of potential concerns. Let’s explore when non-stress tests are recommended during pregnancy:
- High-Risk Pregnancies: Pregnancies deemed high-risk due to maternal or fetal factors often warrant regular NSTs to assess fetal well-being and mitigate potential complications. High-risk conditions may include gestational diabetes, preeclampsia, maternal hypertension, advanced maternal age, multiple gestation (e.g., twins or triplets), intrauterine growth restriction, or a history of stillbirth or pregnancy loss.
- Maternal Medical Conditions: Maternal medical conditions such as diabetes, chronic hypertension, autoimmune disorders, renal disease, or cardiac conditions may necessitate NSTs to monitor fetal responses to maternal health status and ensure optimal outcomes for both the mother and the baby.
- Decreased Fetal Movement: Decreased fetal movement, also known as fetal kick count reduction, is a common indication for NSTs. When expectant mothers perceive a decrease in fetal movements or notice a change in the baby’s activity patterns, NSTs help assess fetal well-being and provide reassurance or prompt further evaluation if needed.
- Post-Term Pregnancy: Post-term pregnancies, defined as pregnancies continuing beyond 42 weeks gestation, pose an increased risk of fetal complications such as oligohydramnios, placental insufficiency, or macrosomia. NSTs may be recommended to monitor fetal well-being and determine the optimal timing for induction of labor to prevent adverse outcomes.
- History of Pregnancy Complications: Women with a history of pregnancy complications, such as previous stillbirth, fetal growth restriction, or placental abnormalities, may undergo regular NSTs in subsequent pregnancies to monitor fetal well-being and reduce the risk of recurrent adverse outcomes.
- Suspected Fetal Growth Restriction: Suspected fetal growth restriction (FGR), characterized by slowed or compromised fetal growth, often prompts NSTs to assess fetal well-being, umbilical artery Doppler studies, and other fetal surveillance methods to guide management decisions and optimize pregnancy outcomes.
- Oligohydramnios or Polyhydramnios: Abnormal amniotic fluid volume, whether decreased (oligohydramnios) or increased (polyhydramnios), may necessitate NSTs to monitor fetal well-being and assess for potential complications such as cord compression, fetal distress, or placental dysfunction.
By recognizing these indications for non-stress tests and incorporating them into prenatal care protocols, healthcare providers can optimize fetal surveillance, detect potential concerns early, and implement timely interventions to promote the health and well-being of both mother and baby. Collaborative decision-making and individualized care plans ensure that NSTs are recommended judiciously based on each patient’s unique clinical circumstances.
Additional Common Questions
-
What is the Purpose of a Non-Stress Test (NST)?
NSTs assess fetal well-being by monitoring the baby’s heart rate in response to its movements. They help healthcare providers evaluate the baby’s health and identify any signs of distress.
-
Is a Non-Stress Test Painful?
No, NSTs are non-invasive and painless procedures. The sensors attached to the mother’s abdomen simply monitor the baby’s heart rate and movements.
-
How Long Does a Non-Stress Test Take?
The duration of an NST typically ranges from 20 to 40 minutes. However, it may vary depending on the specific circumstances and institutional protocols.
-
What Happens if My Non-Stress Test Results are Non-Reactive?
A non-reactive non-stress test in pregnancy result doesn’t necessarily indicate a problem but may prompt further evaluation to assess fetal well-being comprehensively. Your healthcare provider will discuss next steps and any additional tests or interventions that may be needed.
-
Can I Eat or Drink Before a Non-Stress Test?
In most cases, it’s safe to eat and drink normally before an NST. However, your healthcare provider may provide specific instructions based on your individual circumstances.
-
Do I Need to Bring Anything With Me to the Non-Stress Test Appointment?
It’s helpful to bring your prenatal record or any relevant medical documents to your NST appointment. Additionally, wearing comfortable clothing can enhance your comfort during the test.
-
How Often Will I Need Non-Stress Tests During Pregnancy?
The frequency of NSTs varies depending on your medical history, risk factors, and gestational age. Your healthcare provider will recommend an appropriate schedule based on your individual needs.
-
What Should I Do if I Have Questions or Concerns During the Non-Stress Test?
Don’t hesitate to communicate with your healthcare provider if you have any questions or concerns before, during, or after the NST. Your provider is there to address your needs and ensure a positive experience.
Conclusion
As you navigate the beautiful journey of pregnancy, it’s natural to experience a myriad of emotions, questions, and concerns. Among the many facets of prenatal care, non-stress tests (NSTs) stand as beacons of reassurance and confidence, offering tangible evidence of your baby’s well-being and vitality.
Throughout your pregnancy, NSTs serve as invaluable tools in the hands of dedicated healthcare providers, allowing them to monitor your baby’s heart rate patterns and responses to movements. With each NST appointment, you embark on a journey of discovery, witnessing the miracle of life unfolding within you.
As you reflect on the significance of NSTs, remember that these tests are not just about data and numbers—they represent moments of connection and affirmation between you and your precious little one. With each reassuring heartbeat, you’re reminded of the profound love and bond that already exists between you and your baby.
Embrace each NST appointment with confidence and optimism, knowing that you’re actively participating in your baby’s health and well-being. Trust in your healthcare team, ask questions, and advocate for your needs—your voice matters, and your concerns are valid.
As you await the arrival of your little bundle of joy, cherish the moments of anticipation and excitement. Your journey is unique, and every milestone, including NSTs, brings you one step closer to holding your baby in your arms.
So, dear mothers-to-be, embrace the journey with courage, grace, and unwavering faith. Your love knows no bounds, and your strength knows no limits. With each heartbeat, you’re reminded of the incredible gift of motherhood unfolding within you.
Here’s to you, to your baby, and to the beautiful journey ahead. May each NST appointment fill you with reassurance, confidence, and boundless joy.

want to know more
Explore Our Courses










